We have all heard about hepatitis immunization schedule from our friends or family physician. But ever wondered why is it so important? Hepatitis is one of the leading causes of liver inflammation globally and liver cancer – one of the top causes of cancer mortality1. World Hepatitis Day is marked every year on July 28 to raise awareness of the global burden of viral hepatitis.
Every 30 second a person is dying from a hepatitis related illness, with over 1.1 million global mortalities caused by both hepatitis B and C infections2. In India, it is estimated that approx. 45 million people suffer from hepatitis B and 15 million from hepatitis C3. If left untreated, the infection develops into serious illnesses like cancer and liver failure requiring surgery and liver transplants. Timely diagnosis of liver cirrhosis/cancer can lead to better management of the condition and survival rate for the patient. Therefore, it is crucial to create awareness around viral hepatitis, its impact on liver, symptoms and treatment options.
Dr. Abhideep Chaudhary, Senior Director & HOD – HPB Surgery & Liver Transplantation, BLK-MAX Super Speciality Hospital, Delhi, elaborates on the various facets of the disease and its management.
What is hepatitis?
A viral infection that causes inflammation of the liver – a vital organ that filters toxins from our body, breaks down nutrients, produces bile which aids in digestion, among other critical functions. Although there are 5 types of hepatitis namely A, B, C, D and E; Hepatitis B and C are most common cause of chronic hepatitis, both globally and in India.
Symptoms:
• Sudden weight loss
• Loss of appetite
• Nausea or vomiting
• Pain in the abdomen
• Swelling or fluid build-up in the abdomen
• Fever
• Itching
• Yellowing of the skin and eyes
Link between hepatitis and liver cancer
Hepatitis infection is known to damage liver cells and impair its functioning. It can lead to liver cirrhosis, a condition where liver tissue is replaced by scar tissue, which in the long term can progress to primary liver cancer or hepatocellular carcinoma (HCC). Much more common amongst men than women, HCC has high mortality rate. Globally, about 7 lakh deaths are reported due to HCC annually.
A study published in the Journal of Clinical and Experimental Hepatology, found that chronic Hepatitis B virus infection, with tumors developing more often in a cirrhotic (76%) than in a non-cirrhotic liver, is a major factor for HCC development in north Indian population3.
Risk factors for liver cancer:
• Excessive alcohol consumption
• Obesity
• Diabetes
• Genetic metabolic syndrome
• Smoking
• Non-alcoholic fatty liver disease
Treating liver cancer
Accurate diagnosis is critical for right treatment and management of any disease. An ultrasound, MRI or CT scan is utilized to diagnose liver cancer and detect tumors. The therapies with a potential for cure of HCC are surgical resection, percutaneous ablation and liver transplantation.
If cancer cells or tumors are detected, it is of utmost importance to surgically remove the impacted part of liver (hepatectomy) with all tumors to reduce recurrence, improve the patient’s quality of life and survival rate. In advanced cases or if there is associated liver cirrhosis, a liver transplant may be required.
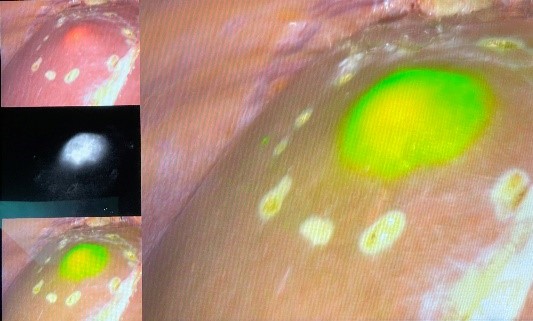
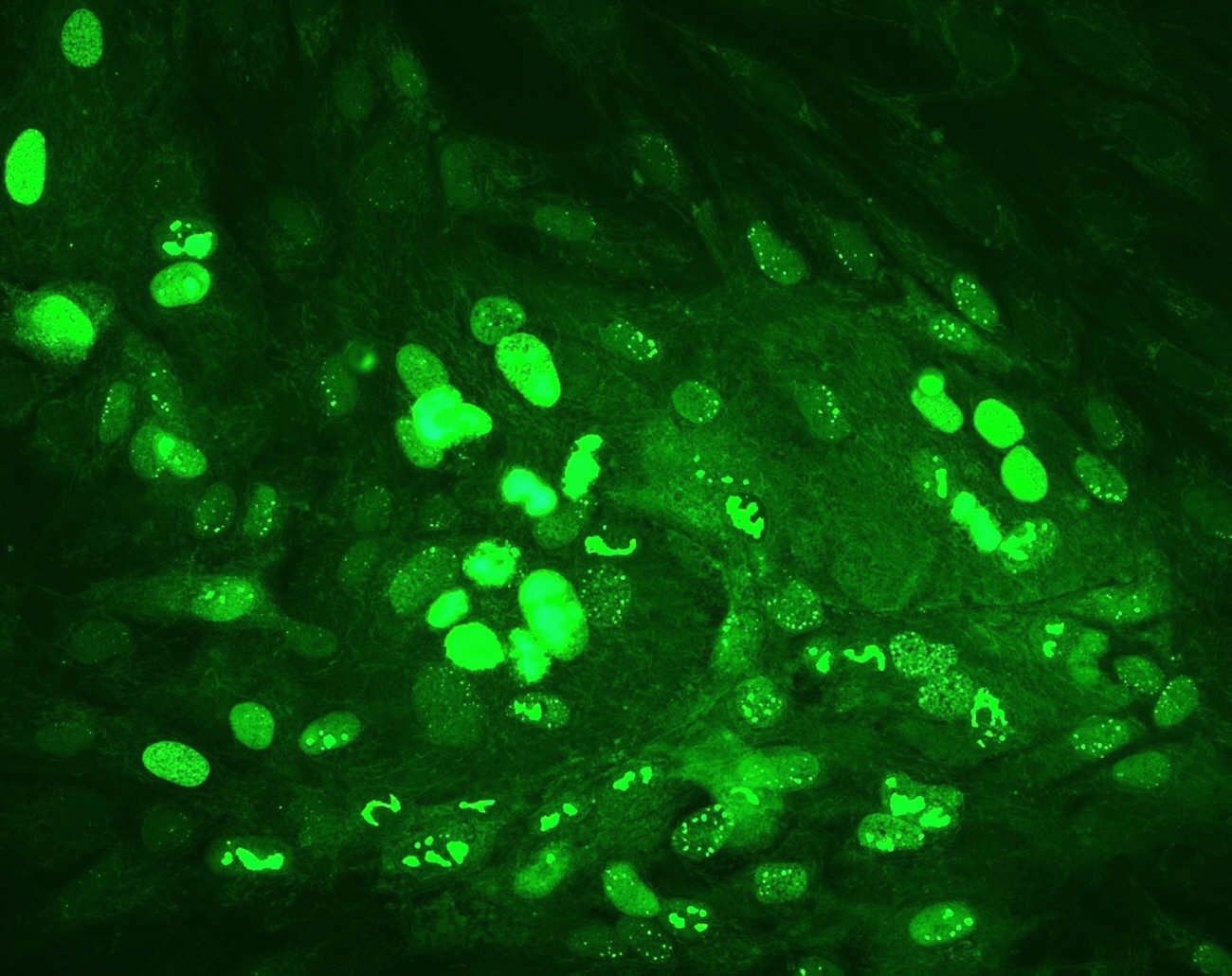
Liver tumor (in green) as seen in the near infrared illumination mode with Fluorescence Imaging technology during surgery. Picture credit: Dr Abhideep Chaudhary
Although conventional diagnostic techniques have been successfully helping surgeons to map tumors for a long time, technological innovations like fluorescence imaging (FI) with indocyanine green (ICG) is revolutionizing liver surgery by allowing real-time tumor visualization and detection of smaller and superficial tumors on the operating table. With a success rate of 94 -100%4, fluorescence guided hepatectomy enables surgeons to achieve greater precision and improve standard of care for patients.
In this procedure, the patient is injected with ICG, a safe and affordable green dye widely used by clinicians across the globe. The cancer cells take up ICG molecules from blood. With the impaired green dye excretion ability, the cells emit fluorescent green colour in the near infrared illumination mode. Thus, assisting surgeons to see, differentiate and selectively remove (liver segmentectomy) the cancer cells from healthy liver tissue during surgery.
Liver segmentectomy is a standard of care in HCC treatment that allows better liver functionality. FI creates clear demarcation line along the liver segment boundary to guide precise removal with minimal blood loss, in comparison to the current blue dye staining technique.
With precision surgery, the chances of tumor recurrence are significantly reduced. As our liver holds the power of regeneration, it recovers to its original weight and shape within few weeks of the surgery.
However, as is said ‘Prevention is better than cure’ – it is time to make responsible, informed choices, lead risk-free life by adopting healthier lifestyle and get timely treatment of viral hepatitis with antiviral drugs. Hepatitis B is one of the major causes of liver cancer and can be prevented by universal immunization against Hepatitis B. Improved sanitation, food safety and immunization are the most effective ways to combat hepatitis A and E. There is a safe and effective vaccine that can protect you from getting hepatitis A.
References:
1. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5394024/
2. https://www.who.int/campaigns/world-hepatitis-day/2021
3. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4284237/
4. Do we need to shift from dye injection to fluorescence in respective liver surgery? Surg Oncol. Published online 2019